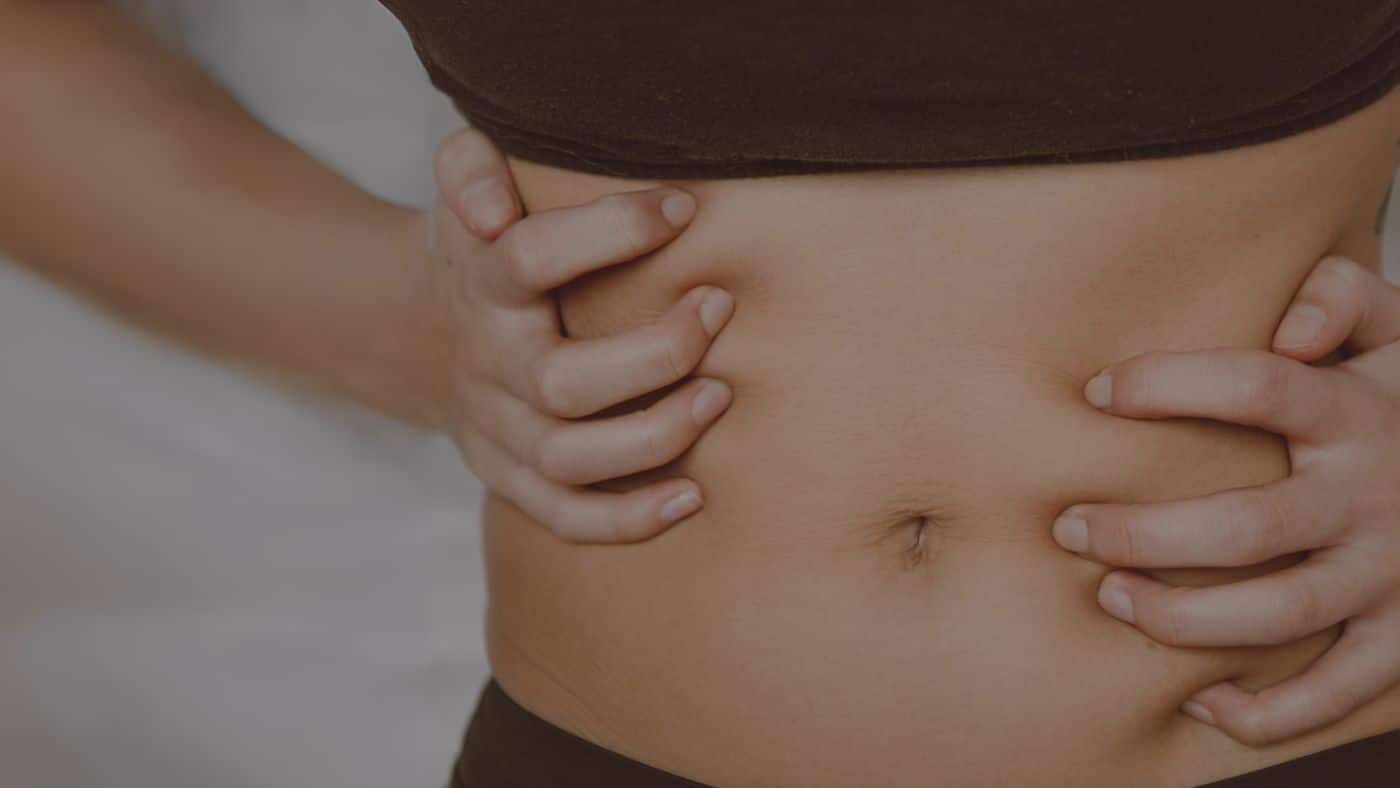
Pay some attention to your gut health, it will be worth it!
The microbiome – the universe within us and its importance for gut health
There are an estimated 250 billion stars in our Milky Way, an unimaginably large number. But the universe inside us is even more impressive: our body is home to around 38 trillion microorganisms, which together form the microbiome. In cellular terms, these microorganisms make up around 50 percent of us and weigh a total of 2-3 kilos. The majority of these microorganisms colonize our gut and form the gut microbiome, which plays a central role in our intestinal health.
The importance of the gut microbiome for gut health
The gut microbiome is crucial for digestion and also regulates our metabolism. There are also microbiomes in the mouth, in the vagina and on the skin that contribute to tissue repair and the immune function of the skin. However, the gut microbiome takes center stage as it influences everything in the body – from metabolic and gut immune function to heart, skin and urogenital health.
Uniqueness of every gut microbiome
Each gut microbiome is unique and constantly changing, influenced by factors such as diet, exercise, medication and sleep. The diversity of strains in the gut microbiome is therefore crucial for optimal gut health.
Dangers for the gut microbiome and gut health
Various influencing factors can damage the intestinal microbiome and thus jeopardize intestinal health. These factors include:
- Antibiotics – They not only kill harmful bacteria, but also beneficial ones.
- Medication and chlorine in drinking water – Even the chlorine present in swimming pools can be harmful.
- Dietary habits – A diet high in meat and fat can promote the growth of harmful bacteria.
- Lifestyle – stress and the consumption of junk food can also have a negative impact on the gut microbiome.
Symptoms of a disturbed gut microbiome
An imbalanced gut microbiome can cause various symptoms that affect gut health, including bloating, nausea, abdominal pain and frequent diarrhea.
The role of probiotics for gut health
Probiotics are living microorganisms which, when administered in sufficient quantities, can promote intestinal health. They support the immune system, produce vitamins and strengthen the intestinal barrier, which leads to improved overall intestinal health.
The role of prebiotics for gut health
Prebiotics are plant fibers, such as inulin, that reach the colon undigested. There, they are fermented by probiotic bacteria and broken down into short-chain fatty acids such as butyrate, acetate and propionate. Prebiotics therefore serve as food for the probiotics or benign intestinal bacteria and thus ensure their growth.
The gut-brain axis and its importance for gut health
The gut-brain axis is a fascinating example of the interactions between our microbiome and our brain. This bidirectional communication pathway enables the gut and the brain to communicate with each other via various biochemical signaling pathways. Disorders in intestinal health can therefore have a direct impact on the brain and vice versa. An unbalanced gut microbiome can send signals to the brain that can lead to anxiety, stress or depression. Conversely, a mental state can also affect the functions of the gut, which further disrupts gut health.
Current research shows that gut flora not only influences our digestion, but can also have profound effects on our mood, appetite, behavior and circadian rhythm. These findings underline the importance of balanced gut health not only for physical but also for mental well-being.
The gut-skin axis and its role in gut health
No less important is the gut-skin axis, which establishes a link between gut health and skin health. Researchers have found that the gut microbiome has a significant influence on skin conditions such as rosacea and acne. This occurs through interactions that can influence inflammatory processes in the skin. A healthy intestinal flora can therefore make a decisive contribution to improving the appearance of the skin and preventing skin diseases.
Maintaining gut health through a balanced diet rich in prebiotic and probiotic foods can therefore have positive effects on overall wellbeing and especially on mental and dermatological health. These axes illustrate how integral gut health is to overall body health and why it is at the center of modern health research and practice.
How stress affects your gut health
Stress has a significant impact on gut health, particularly by impairing the speed of digestion. Under stressful conditions, many people tend to consume more processed foods, which further slows down digestion. This slowdown creates a favorable environment for harmful bacteria to multiply in the gut. Stress also increases the permeability of the intestinal wall, which allows harmful bacteria to pass through the intestinal wall into other areas of the body.
The increased permeability can lead to the loss of the normal microbial biofilm, which in turn weakens the intestinal barrier function. This leads to the release of endotoxins, which trigger systemic inflammation throughout the body. This type of inflammation is particularly insidious as it is often diffuse and difficult to localize, resulting in a range of non-specific symptoms.
These systemic inflammations can also cause dermatological symptoms such as skin irritation, allergies and excessive sebum. This link between stress, gut health and skin condition highlights the importance of a holistic approach to health that takes into account both psychological and physical aspects. Managing stress and promoting healthy gut flora can significantly improve overall health.
Final thoughts on gut health
Investing in good gut health through conscious food choices and possibly taking probiotic supplements such as the LOVE YOUR GUT Daily Biotic Complex from Ogaenics can lead to a healthier life in the long term. It’s important to remember that gut health is an essential part of a comprehensive health strategy. If you want to learn more about gut health, probiotics and the microbiome, read on here:
- How menopause affects your gut health
- Optimize your gut health with synbiotics
- Skin problems? The gut-skin axis is behind it
- Irritable bowel syndrome: Vitamin D can banish flatulence
- How the microbiome influences our health and ageing
- Bloated belly while traveling: how to prevent it
- What you should look for in a probiotic
- What can I expect when I take probiotics?
Store probiotics
-
Bestseller
Love Your Gut
Bio Daily Biotic Complex Premium for the gut: 21 bacterial strains plus organic fiberab 29,90 € -
Set 2x Love Your Gut | Daily Biotic Complex
Set of 2 Bio Daily Biotic Complex Premium for the gut: 21 bacterial strains plus organic fiber94,90 €99,80 €1.176,89 €1.119,10 € / kg
(1) Hill, C., Guarner, F., Reid, G. et al. The International Scientific Association for Probiotics and Prebiotics consensus statement on the scope and appropriate use of the term probiotic. Nat Rev Gastroenterol Hepatol 11, 506-514 (2014).
(2) Bowe, W.P., Logan, A.C. Acne vulgaris, probiotics and the gut-brain-skin axis – back to the future? Gut Pathog 3, 1 (2011).
(3) Matenchuk, Brittany A et al. Sleep, circadian rhythm, and gut microbiota. Sleep medicine reviews vol. 53 (2020): 101340.
(4) Del Piano, Mario et al. “The use of probiotics in healthy volunteers with evacuation disorders and hard stools: a double-blind, randomized, placebo-controlled study.” Journal of clinical gastroenterology vol. 44 Suppl 1 (2010): S30-4






 No products in the cart.
No products in the cart.